Table of Contents
That “blocked ear” feeling can be surprisingly stubborn. Sometimes it shows up as fullness, popping, crackling, muffled hearing, or a sense that your own voice sounds louder than it should. It often arrives after a cold, during allergy season, after a flight, or seemingly for no clear reason at all. The frustrating part is that the same sensation can come from very different causes. Wax in the ear canal can do it. So can pressure imbalance behind the eardrum. So can fluid in the middle ear. So can inflammation after an infection. If you treat the wrong cause, you usually waste time and patience. Tympanometry exists to stop that loop. It is a quick, objective test that measures how the eardrum moves and what the pressure is doing in the middle ear. In practical terms, it helps separate “the ear canal is blocked” from “the middle ear isn’t ventilating properly” and points you toward the right next step without guesswork.
Why “blocked” ears often have nothing to do with wax
Most people picture the ear as a tube that gets clogged. In reality, the “blocked” sensation is often a pressure story. The middle ear is an air-filled space sealed by the eardrum. It connects to the back of the nose via the Eustachian tube, which opens briefly when you swallow, yawn, or chew. That tiny opening equalises pressure and helps the middle ear stay aerated. When the nose and throat lining is swollen, after a viral cold or during allergies, the Eustachian tube can become sluggish. Pressure can drop or build behind the eardrum, changing how it sits and how it vibrates. The result is a very real sensation of fullness and muffled sound, even when the ear canal is perfectly clear. In other cases, fluid can collect behind the eardrum, particularly after a cold. This can also feel like “cotton wool” hearing. Wax is still common and can absolutely cause the same symptom, but it is only one chapter of the story. The point is that your ears can feel blocked for more than one reason, and the right treatment depends on which reason is actually present.
What tympanometry measures
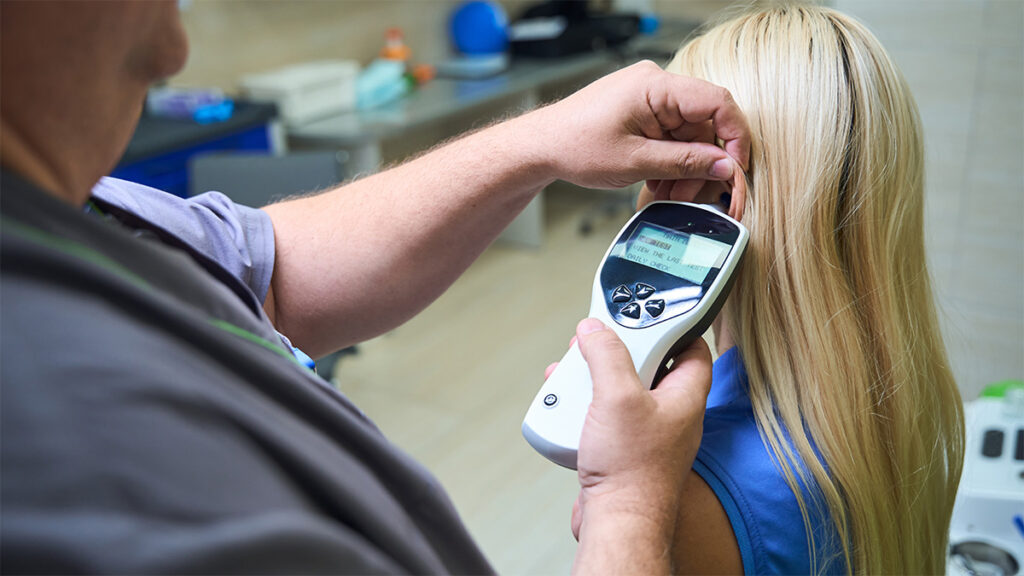
Tympanometry is a test of middle ear function. It uses a small probe tip that seals gently in the ear canal for a few seconds. The device changes the air pressure very slightly and plays a tone. As pressure changes, the eardrum moves more or less. The tympanometer measures that movement, along with the ear canal volume between the probe and the eardrum. The output is a tympanogram, a curve that reflects how the middle ear system is behaving. Clinically, tympanometry provides quantitative information about the likelihood of fluid behind the eardrum, how mobile the eardrum is, and whether middle ear pressure is unusually negative or positive. It does not replace a clinician looking inside the ear. It complements it. A healthy approach is to combine history, otoscopy, and tympanometry, because a curve makes more sense when it matches what we can see and what you are feeling.
What the main tympanogram patterns usually mean
You do not need to memorise curves, but understanding the broad patterns helps you see why tympanometry is useful. A “Type A” pattern is generally considered within the expected range: the eardrum moves well and pressure is near normal. If your ear feels blocked and the tympanogram is Type A, we start thinking about other contributors, such as wax or canal irritation that was seen on otoscopy, sound sensitivity changes, jaw tension, or non-ear factors that can mimic fullness. It can also be reassuring, because it suggests there is no clear middle ear pressure problem driving your symptoms. A “Type C” pattern typically suggests negative middle ear pressure. This is commonly linked with Eustachian tube dysfunction, often after colds or during allergy flares. Many people with Type C describe popping, crackling, and intermittent fullness that changes through the day or with altitude. A “Type B” pattern is usually flatter and commonly associated with reduced eardrum mobility, often because fluid is present behind the eardrum. This can produce more constant muffling. Importantly, tympanometry can also help interpret special situations. For example, if someone has a ventilation tube in place or a perforated eardrum, the ear canal volume and curve behaviour can point in that direction. None of these patterns automatically dictate a single treatment, but they quickly narrow the field. That is the value. They turn “blocked ears” from a vague complaint into a more specific middle ear picture.
What the test feels like and what it does not do
Tympanometry is usually brief and well tolerated. You may feel a gentle pressure change, similar to driving up a hill, and you will hear a tone. It can feel slightly odd but should not be painful. If the ear canal is very sore, inflamed, or completely blocked with wax, the test can be uncomfortable or unreliable, which is why otoscopy is typically done alongside it. One practical note is that the test requires a good seal, so if the probe cannot seal properly, the results may not be meaningful. That is not a failure, it is information. It tells the clinician to address the ear canal first or to interpret results cautiously. Tympanometry also does not diagnose everything. It does not measure nerve hearing or speech understanding. It is a middle ear pressure and mobility tool. If your main issue is speech clarity, or if your hearing concerns are broader, tympanometry is one piece of a larger assessment, not the entire assessment. The strength of the test is its objectivity and speed when the question is, “Is this a canal issue, or is the middle ear under pressure or carrying fluid?”
Why it changes the next step so quickly
In real life, people tend to try whatever feels intuitive. Ear drops for a blocked sensation. Repeated “popping” manoeuvres. Nasal sprays used without a clear plan. In some cases, these steps are harmless but ineffective. In others, they can irritate the ear canal or lead to overuse of decongestant sprays. Tympanometry helps choose the right direction early. If the issue is wax, the plan focuses on safe wax management and avoiding cotton buds, not pressure manoeuvres. If the issue is negative middle ear pressure, the plan often focuses on the nose and Eustachian tube, supporting ventilation and addressing allergy or post-viral inflammation rather than treating the ear canal. If fluid is likely, management depends on duration, symptoms, and risk factors. In children, fluid after a cold often resolves. In adults, persistent one-sided fluid or persistent unilateral symptoms deserve careful assessment, and ENT input may be appropriate depending on the clinical picture. Tympanometry does not replace clinical judgement, but it makes the judgement more informed. It also helps people feel calmer, because a symptom that feels mysterious becomes measurable. That is very much in line with Audiocare’s philosophy: calm assessment, clear explanation, and a plan that fits the person rather than a one-size approach.
When to book a check
If ear fullness or popping lasts more than a few days, keeps returning, or comes with persistent muffled hearing, it is worth booking a review. It is also worth booking if one ear consistently feels different from the other. One-sided symptoms deserve a proper comparison and a clear look inside the ear. Seek prompt medical care if you have severe ear pain, high fever, discharge from the ear, sudden hearing loss, significant spinning dizziness, or swelling around the ear. Those are not “wait and see” situations. For the more common scenario of pressure and muffling after a cold or allergy flare, a calm check with otoscopy and tympanometry can clarify the cause quickly, stop unnecessary self-treatments, and point you toward the simplest effective next step.
A fast test, a clearer plan
Blocked ears feel deceptively simple, but they are not always caused by the same thing. Tympanometry is one of the most practical tools we have because it measures what you cannot see or feel directly: middle ear pressure and eardrum mobility. Combined with a clear look in the ear canal, it helps separate wax from pressure, pressure from fluid, and uncertainty from a plan. If your ears keep feeling full, popping, or muffled, booking a quick review can save you weeks of guessing. At Audiocare, that review is designed to be calm, objective, and useful, with clear explanations and practical next steps that fit your situation.
References
- https://www.thebsa.org.uk/wp-content/uploads/2026/03/BSA-Recommended-Procedure-Tympanometry-Acoustic-Reflex-Thresholds-March-2026-minor-revision.pdf
- https://www.nhs.uk/conditions/earwax-build-up/
- https://www.nhs.uk/conditions/ear-infections/
- https://my.clevelandclinic.org/health/diagnostics/24222-tympanometry
- https://audiocare.pt/advanced-tympanometry-services/









